Tirsdag 29. april i Trondheim skal undertegnede snakke på Dataforeningens fagmøte om et aktuelt tema: Er det i det hele tatt mulig å lage løsninger som er både sikre og brukervennlige?
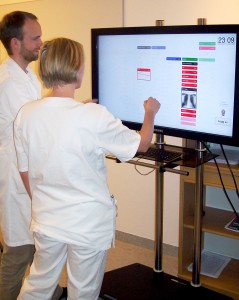
I en rykende fersk forskningsartikkel publisert i tidsskriftet BMC Medical Informatics and Decision Making (fri tilgang), beskriver vi utviklingsarbeidet og resultatene fra eksperimentering med en digital tavleløsning for sykehus. Hvordan kan digitale tavler brukes til statusoppdateringer med potensielt sensitiv informasjon, men samtidig gjøre fordel av tavlens synlighet på en vegg som mange kan se?
Kom på Dataforeningens nettverksmøte i Trondheim, tirsdag 29. april kl 1730, og hør mer om både dette prosjektet og tematikken for øvrig!
Erlend Andreas Gjære and Børge Lillebo:
Designing privacy-friendly digital whiteboards for mediation of clinical progress
BMC Medical Informatics and Decision Making 2014, 14:27.
Background: In hospitals, digital versions of dry-erase whiteboards are increasingly becoming more common. One of the purposes with such whiteboards is to support coordination of care by augmenting visibility and availability of clinical information. However, clinical information usually concerns patients and is regarded as sensitive personal health information, meaning that it should be access controlled. The purpose of this study is to explore how digital whiteboards can be designed for supporting coordination of care, by providing clinicians with useful information in a usable way, and at the same time protect patient privacy.
Methods: A demo application was designed, demonstrated and evaluated iteratively. In total, 15 professional ward nurses role-played a scenario in which the application played a central part. Afterwards, the participants were interviewed. All interviews were recorded, transcribed verbatim, and analysed qualitatively.
Results: The participants valued having updated clinical information presented on a digital whiteboard, even if the information was de-identified and abstracted. According to the participants, such information could possibly improve inter-departmental communication, reduce the number of electronic health record-logins, and make nurses more rapidly aware of new information. The participants expected that they would be able to re-identify much of the de-identified information in real situations based on their insight into their patients’ recent and expected care activities. Moreover, they also valued being able to easily access more detailed information and verify patient identities. While abstraction and de-identification was regarded to sufficiently protect the patients’ privacy, the nurses also pointed out the importance of having control over what can be seen by other patients and passers-by if detailed medical information was accessed on a digital whiteboard.
Conclusions: Presenting updated information from patient care activities on a digital whiteboard in a de-identified and abstracted format may support coordination of care at a hospital ward without compromising patient privacy.
